I work with residents daily. I get to see how their practice has been molded by other attending anesthesiologists and their peers. I wonder some time, “where did this come from, or who is teaching this?”
I view having to give vaso-pressors as a failure.
I see it as a failure, because, it means that I missed something.
The three most common reasons for hypotension after the induction of anesthesia are:
- Too much anesthesia
- Too much anesthesia
- Too much anesthesia
Other reasons include:
- Hypovolemia (the fourth most common reason)
- Frailty
- Traumatic shock
- A compromised vascular system (pump failure or malfunctioning conduction system)
- Anemia (lack of plasma viscosity)
- Sepsis
- Spinal shock
I suspect few would argue that (non-deliberate) hypotension is beneficial. Yet, hypotension and its treatment with vaso-pressors after the induction of anesthesia is so common, yet so unnecessary.
I’m guilty. Whenever I fail to watch trainees carefully and control the amount of anesthesia given, I estimate that half of the patients will receive a vaso-pressor owing to “too much anesthesia.”
It is a cycle of:
- Give too much anesthesia
- Give a vaso-pressor
- Turn down the anesthesia,
that stems from the knee-jerk response of overdosing with pre-induction opioid, propofol, and finally 2-3% sevoforane. I guess this cycle stems from a desire to prevent re-call.
Is it really necessary to load in opioids and turn the sevoflurane up to 2-3% while the propofol has not yet redistributed? Isn’t it just as effective to hold off on the opioid and keep the sevoflurane concentration to amnesic levels (0.5-1%) during the prepping and draping while there is no stimulation?
Minimum alveolar concentration (MAC), the concentration at which 50% of patients do not respond to surgical incision, is 2.6% (25 years of age) for sevoflurane.
Surgical levels of anesthesia are generally achieved with concentrations between 0.5% to 3%.
The concentration at which amnesia and loss of awareness occur (MAC – awake) is 0.6%.
Surgical levels of anesthesia are generally achieved with concentrations between 0.5% to 3%.
MAC is reduced in the elderly (50% reduction by age 80).
Following IV bolus administration, propofol’s CNS actions are terminated by redistribution from the brain to other compartments. This process occurs with a redistribution halftime in the 2-8 minute range.
I have no need to pre-load opioid, or do I rush to get the sevoflurane up to 2-3%, both of which are not necessary until there is an incision. The upside to this approach is that the patient will not be over anesthetized and will likely be normotensive. The downside is that the patient may move or cough if stimulated. Unless the operation is really quick (rare in my experience) and does not require muscle relaxation, I prevent movement/cough with vecuronium, given immediately after intubation and before return of the twitch (see: https://trauma01.wordpress.com/2012/03/14/do-not-wait-for-return-of-twitch-after-succynilcholine/).
This way, I have a patient who is immobile but amnesic and normotensive.
Now, I pay attention to what the surgeons are doing and I anticipate and prevent the normal hyperdynamic response to surgical stimulation by turning up the sevoflurane (with high flows if I want to get there quickly), and by titrating opioid, as required. Even with this “minimalist” approach, some patients (in particular, trauma victims, frail elderly, those with hypovolemia) will be hypotensive. Depending on the degree of hypotension, a pressor might be indicated. In these cases, the most likely cause of the hypotension is hypovolemia and the treatment for that is fluid.
Are pressors bad? I believe they are, in most cases. Can I show that they are bad with so-called “evidence based medicine.” No, I can not. But, I’ll offer my opinion as to why I think they are bad.
The four most common causes of hypotension after induction of anesthesia are: 1-3, too much anesthesia, and 4, hypovolemia. Too much anesthesia means that we have so deeply anesthetized the patient that we have eliminated the catecholamines that were maintaining normotension before induction. Too much anesthesia is especially bad in the patient who is secreting high levels of catecholamines to compensate for hypovolemia.
Hypotension from too much anesthesia and owing to lower catecholamine levels is most likely due to veno- and arteriolar-dilatation as well as decreased inotropy and chronotropy. The major culprit here is venodilation, which causes decreased venous return leading to decreased stroke volume and decreased cardiac output. Arteriolar dilatation contributes to the hypotension by decreasing vascular resistance. The blood pressure is low because the cardiac output and vascular resistance are decreased.
Phenyleprhine, the most used vasopressor in this situation, will return the blood pressure to normal. Is that bad? I’m not sure. Does it produce a normal blood pressure by improving venous return, cardiac filling, stroke volume, cardiac output, and peripheral vascular resistance? Probably not. Since phenylephrine is mostly an alpha agonist, it likely produces a higher blood pressure by increasing after-load. Is an empty heart working against a high resistance the treatment of choice? I doubt it.
It is said, “The dumbest kidney is smarter than the smartest doctor.” I believe the same is true for the vascular system of the patient who is not over anesthetized. The vascular system of the adequately (but not overly) anesthetized patient will deliver the appropriate catecholamine to the appropriate sites to maintain normotension better than the smartest anesthesiologist can.
If a pressor is necessary, perhaps one with mixed alpha/beta actions (ephedrine) is more physiological and appropriate.
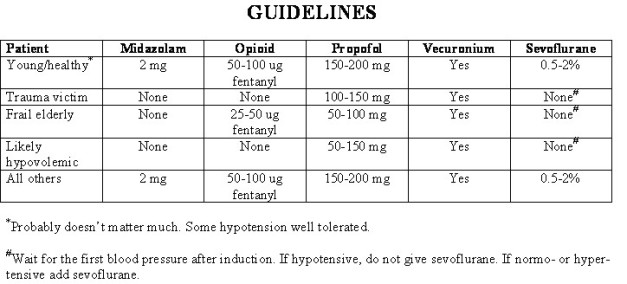
So, what do I suggest?
In regard to recall, it is my belief that hypotensive patients don’t have recall. The hypotensive patient is probably too deeply anesthetized to have recall. The two patients (in 35 years) that I have had with recall, both had hypertension and tachycardia.
As the end of the operation nears, I begin considering how tissue damaging the operation is and how much pain the patient might have. Generally minimally invasive operations (lap appy, lap cholecystectomy, lap ectopic pregnancy) and other operations where the surgeon has injected local anesthesia will not require much narcotic. Certainly not more than 250 ug of fentanyl given during the operation. Long acting narcotics like hydromorphone are usually unnecessary for these operations. Post-operative pain varies considerably from patient to patient. For the same operation, some have little pain, while others have a lot. Rather than give too much narcotic and prolong emergence, it is better to wait until the patient is extubated and then give the right amount of narcotic to manage the pain.
In summary, this is “A Philosophy.” It is not a science.